Stroke Rehabilitation
Hemiparesis, Hemiplegia and other Motor Weaknesses
Hemiparesis and hemiplegia are inherently unpredictable and challenging, with symptoms changing over time. Adequate intervention, including extensive physical therapy, can substantially improve the chances of a full recovery but results can be attained only if extensive therapy is applied; if activities chosen are meaningful, occasionally modified and customised.
Hemiparesis (or unilateral paresis) and Hemiplegia are nervous system disorders. While hemiparesis refers to weakness on one side of the body, hemiplegia is a paralysis that affects one side of the body. An injury can produce both symptoms at different times making it difficult to treat. An injury to the spinal cord or brain interferes with the body’s ability to send or receive signals to the region of the body affected by the injury. The affected side is usually the opposite of the side of the brain being injured (injury to the right side of the brain - affects the left side of the body).
Most prevalent causes of both disorders are mild to moderate nerve or brain damage, often related to strokes, infections, brain injuries or spinal cord injuries, which affect the central nervous system (CNS). Hemiparesis or hemiplegia may develop in a region of the brain that affects movement or perception. The most common cause of both injuries is a stroke. Other causes for the condition are possible:
- Damage to the neurons due to a degenerative disorder such as Parkinson’s or MND
- Brain infections such as meningitis
- Brain cancer or lesions
- Traumatic injuries, such as a blow to the head during a car accident
- Congenital disorders such as cerebral palsy
Stroke
Stroke is a broad term that refers to cerebrovascular accident, blood vessels (artery) that supply the blood (oxygen) to the brain become blocked or begin to bleed (National Stroke Audit, 2016, National Australian Stroke Foundation). There are three types of stroke; cerebral haemorrhage, cerebral infarction and Transient Ischemic Attack (TIA). A haemorrhagic stroke is a bleed in the brain, an infarction (also known as ischaemic stroke) is caused by a blockage, such as a blood clot or a fatty plaque, in the artery supplying the brain. TIA (also called a “mini stroke”) is caused by a temporary clot and does not cause permanent disability, however, it can be a warning sign pointing to a more serious stroke about to happen. Therefore, urgency in treatment is essential as the brain damage, due to the lack of oxygen may be more permanent.
Ischaemic stroke is more common, accounting for 80% of stroke incidents (National Stroke Foundation 2012). According to Australian Bureau of Statistics (ABS) for 2015, stroke is the third leading cause of death in Australia, with 10,869 fatalities and mostly affecting individuals 65years of age and older.
Evaluation
Symptoms of hemiplegia: difficulty moving one side of the body and loss in sensation on that side, keeping one hand in a fist, difficulty swallowing or with speech, breathing difficulties, difficulty with bowel or bladder control. Movement dissociation (selective disorder) may occur in one of the three forms of the movement: voluntary, automatic and reflex. The ability to isolate movement at specific joints is crucial for most activities. Weakness of the hand, foot, shoulder, and hip is the most frequent motor-deficit profile. (Footnote: Arboix, A. & Marti-Vilata, J. L. (2012) Hemiparesis and other types of motor weakness, In L. R. Caplan & J. van Gijn (Eds.), Stroke Syndroms 3rd ed, Cambridge University Press. ) The main cause of motor weakness is damage to the primary crossed corticospinal tract. Therefore, common symptoms are difficulties with motor skills and weakness in large areas on one side of the body (e.g. difficulty lifting arms). Examination is usually administered to rule out other causes, such as: muscle strains, pinched nerves or loss of blood flow.
The evaluation of Hemiparesis may involve Fugl-Meyer Assessment (FMA) scale to assess the sensorimotor impairment in individuals who have had the stroke (Footnote: Fugl-Meyer Assessment. Fugl-Meyer, A., Jääakö, L., Leyman, I., Olsson, I., & Steglind, S. (1975). The post-stroke hemiplegic patient. Part I. A method for evaluation of physical performance. Scandinavian Journal of Rehabilitation Medicine, 7, 13–31. ) Pusher syndrome may develop and cause a person to shift their weight to the affected side, which makes movement painful and also reduces motor skills. The assessment of the severity of pusher syndrome can be achieved by Functional Reach Test.
The Chedoke-McMaster Stroke Assessment (CMSA) measures two components evaluating motor impairment and disability. (Footnote: Chedoke-McMaster Stroke Assessment (CMSA). Gowland, C., Stratford, P., Ward, M., Moreland, J., Torresin, W., Van Hullenaar, S., . . . Plews, N. (1993). Measuring physical impairment and disability with the Chedoke-McMaster Stroke Assessment. Stroke, 24, 58–63. ) The Stroke Rehabilitation Assessment of Movement (STREAM) measures voluntary movements and general mobility.
 |
Treatment for Hemiparesis and Hemiplegia
Though hemiparesis and hemiplegia produce different symptoms, they are substantially similar in cause and treatment. Neither of them is a progressive disorder (unless result of a brain tumour), therefore, recovery is possible. However, due to lack of mobility, other complications may occur. To treat either condition, a doctor will first look at what caused the symptoms and then decide which treatment would work the best. When a stroke is the cause, the damage may not be reversed, but a number of treatments will help restore some or even most functioning. Rehabilitation is recommended to regain maximum function and quality of life and usually it is in some form of occupational therapy. It is crucial that patients include some form of rehabilitation to improve their condition.
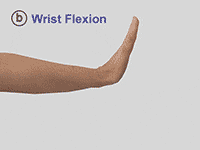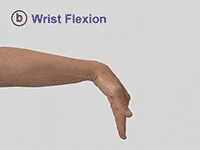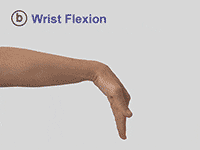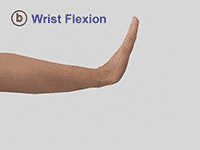
Spasticity following a stroke occurs in about 30% of patients, so to determine its magnitude neuroimaging is essential. Some of these patients develop spasticity within first six weeks after the stroke and most of them affect the elbow, wrist and the ankle. (Footnote: Wissel, J., Verrier, M., Simpson, D. M., Charles, D., Guinto, P., Papapetropoulos, S., & Sunnerhagen, K. S. (2015). Post-stroke spasticity: predictors of early development and considerations for therapeutic intervention. PM & R: the journal of injury, function, and rehabilitation, 7(1): 60-67. ) In the upper limbs, the most frequent pattern of arm spasticity is internal rotation and adduction of the shoulder coupled with flexion at the elbow (fig.2), the wrist and the fingers (fig 3.).
 |
 |
A high degree of paresis and hypoesthesia at stroke onset are identified as one of its predictors. Spasticity affects the quality of life, induce pain, ankylosis, muscle weakness but it also reduces the effects of rehabilitation (fig 1).
Nelles and collegues demonstrated, by using Positron Emission Tomography (PET) scans, a correlation between the movement recovery in patients with hemiparesis and increase of brain metabolism in the parieto-premotor areas (Footnote: Nelles, G., Jentzen, W., Jueptner, M., Mu¨ller, S., & Diener, H. C. (2001). Arm training induced brain plasticity in stroke studied with serial positron emission tomography. Neuroimage, 13: 1146–1154.71. )
Struppler and his team also showed (PET scans) that the improvement in a motor task, most specifically finger extension, was related to an increase of neural activation in parieto-premotor areas, which is known to be interrelated to motor areas which control arm and hand movements. Further, an additional increase of the brain metabolism was also observed in the SMA and CMA. (Footnote: Struppler, A., Binkofski, F., Angerer, B., Bernhardt, M., Spiegel, S., Drzezga, A., & Bartenstein, P. (2007). A fronto-parietal network is mediating improvement of motor function related to repetitive peripheralmagnetic stimulation: A PET-H2O15 study. Neuroimage, 36(Suppl 2):T174–186. )
For example, constraint-induced movement therapy (CI Therapy), Mirror Therapy (MT) or extensive Awareness Drawing Therapy (ADT) are very beneficial. After the stroke most people avoid using impaired limbs, behaviour called learned non-use. They rely on their unaffected side but if an arm or hand is paralysed, it is crucial to improve its function by treating it as normally as possible and not neglecting it. CI movement therapy usually consists of constraining the unaffected side, which forces the brain to adjust and rebuild, or in some cases even create new neural pathways. Mirror therapy uses the unaffected limb to stimulate motor function of the hemiparetic limb, in which the mirror is used to “trick” the brain. (Footnote: Thieme, H., Mehrholz, J., Pohl, M., Behrens, J., & Dohle, C. (2013). Mirror therapy for improving motor function after stroke. Stroke, 44: 1-2. )
Drawing Awareness Therapy is in this sense similar to CI therapy, as it employs constraints (if necessary) of the healthy arm, and at the same time requires concentration and awareness during exercises, which helps with deep elaborate learning, strengthens the new neural pathways and improves motor coordination. (Footnote: Chamberlain, R., McManus, C., Brunswick, N., Rankin, Q., Riley, H., &Kanai, R. (2014). Drawing on the right side of the brain: A voxel-based morphometry analysis of observational drawing. NeuroImage, 96: 167- 173 )
An example: After constraining the healthy arm place the affected limb on the white paper where it can be seen (this is important if the person lacks awareness) then feel the pencil between your fingers. Let your fingers (use your palm too) play with the pencil. Then, while being fully concentrated on every movement, connect the dots (already placed on the piece of paper) by drawing deliberate continuous lines (without breaking your wrist) in a direction asked of you by your therapist. Drawing exercises are created for different purposes: drawing for the exercises of shoulders and elbows, or for the fine motor control skills – wrist and finger exercises. Each exercise is devised for a specific task that requires certain skills to be acquired, hence to force the brain to adjust. Furthermore, effects of drawing exercises are magnified if motor imagery is introduced. As noted by Hy and his colleagues, gait training with motor imagery training significantly improved the balance and gait abilities of chronic stroke patients, in comparison to gait training alone. (Footnote: Cho, H., Kim, J. S., & Lee, G. C. (2013). Effects of motor imagery training on balance and gait abilities in post-stroke patients: a randomized controlled trial. Clinical rehabilitation, 27(8): 675-80. ) When investigating whether motor imagery training improves hand function in chronic stroke patients, Dijkerman et al.(2004) demonstrated that patients improved on many tasks but imagery alone without supervision may improve performance on the trained task only. (Footnote: Dijkerman, H. C., Ietswaart, M., Johnston, M., & MacWalter, R. S. (2004). Does motor imagery training improve hand function in chronic stroke patients? A pilot study. Clinical rehabilitation, 18(5):538-49. ) Even though extensive research demonstrates that supervised training sessions are extremely beneficial in treating hemiparesis and other motor weaknesses, not many established rehabilitation centres incorporate those therapies into their programs, and too often patients are released without any aftercare treatment plans.
Another treatment that has shown results is Guided movement therapy. Therapist should choose activities that have meaning to the person to encourage participation. It is similar to Drawing Awareness Therapy but the therapist places a hand over the person’s hand to help him/her correctly manipulate objects during a task. Affected upper extremity should be positioned in shoulder protraction, while arm is brought forward, spine aligned, and finger extended. When sitting, both feet should be flat on the floor and both arms supported on a table or on armrests. (Footnote: Gilmore, P. E., Spaulding, S. J., & Vandervoort, A. A. (2004). Hemiplegic Shoulder Pain: Implications for Occupational Therapy Treatment. Canadian Journal of Occupational Therapy, 71 (1): 36-46. )
Therapeutic electrical stimulation (TES) has demonstrated some short-term improvement in arm function and range of motion, subluxation and pain reduction; however, evidence is inconclusive for long-term benefits. (Footnote: Aoyagi, Y., & Tsubahara, A. (2004). Therapeutic orthosis and electrical stimulation for upper extremity hemiplegia after stroke: A review of effectiveness based on evidence. Topics in Stroke Rehabilitation, 13(3), 9–15. )
Physical, occupational, or exercise therapy, be it CI therapy or extensive Drawing Awareness Therapy may restore functioning and help the brain work around the injury and therefore, increase and support later independence. It can be achieved even if the injury is not recent. Furthermore, psychotherapy is welcomed to address the psychological impact of a severe injury. Alternative treatments such as acupuncture and dietary changes are also helpful.
Prognosis and aftercare
Hemiparesis and hemiplegia are inherently unpredictable and challenging, with symptoms changing over time. Adequate intervention, including extensive physical therapy, can substantially improve the chances of a full recovery but results can be attained only if extensive therapy is applied; if activities chosen are meaningful, occasionally modified and customised. Psychotherapy is also important, since the overwhelming nature of these injuries can interfere with the patient’s motivation in the absence of immediate improvements. Many hospitals that have specialised units dedicated to stroke, either‘ comprehensive stroke centre’ or ‘primary stroke centre’, significantly improve the recovery of stroke patients. There are various types of stroke units, with different range of functions and services available—acute stroke units, comprehensive stroke units and stroke rehabilitation units.
However, due to limited resources most stroke units offer short-term rehabilitation programs and struggle with the continuity of adequate care for stroke patients. Those patients can benefit from further rehabilitation even years after the event of stroke.
Drawing Therapy Centres provide a range of therapies aimed at helping individuals regain their physical capacity needed to remain in their own homes and improving their quality of life. In accordance with National Stoke Audit’s recommendations they also commonly provide psychological assessments and support.



















Leave a Comment